What is Glaucoma?
Glaucoma is a condition in which the optic nerve suffers progressive damage with loss of nerve fibres, resulting in progressive loss of vision. The condition is commonly due to raised eye pressure over a long period.
The eye produces fluid constantly, which is drained away through a sieve-like structure called the Trabecular Meshwork at the inner corner between the cornea and the iris. When the resistance within the trabecular meshwork builds up, this will cause a build-up of pressure inside the eyes. The pressure will cause damage to the optic nerve head (optic disc) and result in the loss of vision.
How do you know that you have glaucoma?
Most patients with glaucoma do not have any symptoms. Usually, opticians detect possible glaucoma changes with raised eye pressure, suspicious optic nerve head (optic disc), or visual field loss during routine eye tests. Patients may notice reduced vision when visual field loss becomes more advanced in both eyes.
Some patients who suffer from acute angle closure glaucoma will get symptoms with eye pain, blurred vision, headache or browache and seeing 'halos' around lights at night.
Who are at risk of glaucoma?
Around 60 million people worldwide suffer from glaucoma. In UK, it has been estimated that 50% of people with glaucoma are not diagnosed.
The following groups of people have increased risks of glaucoma:
- Older age (>50 yr old)
- Family history of glaucoma (especially in first degree relatives)
- African Caribbean ethnicity
- Extreme short and long sighted people
- Diabetic patients with poor sugar control
How is glaucoma monitored?
Glaucoma is mainly monitored by the following tests:
Eye pressure measurement
Normal eye pressure is between 8 and 21 mmHg. If the pressure is persistently raised above 21 mmHg, there is an increased risk of glaucoma. The higher the pressure, the higher the risk of glaucoma. In some patients, however, even if the eye pressure is within the normal range, they can still develop glaucoma because their optic nerves are more vulnerable and require a much lower eye pressure to reduce the risk of further glaucoma damage.
Eye pressure is commonly measured using an applanation method. After instilling anaesthetic eye drops, a small Goldmann-type applanation tonometer is widely used with the slit-lamp to measure eye pressure. The newer rebound tonometer (iCare) or non-contact tonometer can be used when patients cannot tolerate the applanation method,
Eye pressure daytime phasing is performed when the glaucoma specialist suspects the patient's eye pressures fluctuate widely throughout the day. This may be causing optic nerve damage without demonstrating raised eye pressure during serial measurements in the clinic. Patients attend the outpatient department for a whole day of eye pressure testing every 2 hours between 9:00 a.m. and 5:00 p.m. Some clinics can lend patients a home tonometer to measure the pressure throughout the day at home and then return the tonometer to the clinic to download the readings.
Visual field test
The visual field test measures central and peripheral vision sensitivity. It involves sitting in front of a dome-shaped machine. Light spots of different brightness shine on the inner surface of the dome. You are instructed to look straight ahead at a target and press a button when you can see the light spots against a bright background.
The picture shows a typical visual field defect (black area) due to glaucoma damage. Patients may not notice the visual field defects at the early stage of glaucoma because the other eye tends to compensate for losing vision in some areas. However, the loss of visual field in both eyes may affect the exact location when the disease progresses. Patients may start to notice that they are not seeing well in some areas, or objects or cars appear unexpectedly in the remaining centre of vision.
Driving can become difficult when there is significant visual field loss in both eyes. Patients must inform DVLA when they are diagnosed with suffering from glaucoma. Patients will need to complete a V1 form, and DVLA will arrange a visual field test for you to do with both eyes open. The DVLA will decide whether you meet the visual standard for driving based on the field test results.
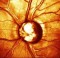
Optic nerve head (Optic disc)
Optic disc is the optic nerve head that we can see inside the eye with a special focusing lens. In normal people, there is a small depression on the optic disc called the optic disc cup. This is normally occupying 30% of the optuc disc area and the doctor normally measure the vertical cup-to-disc ratio during routine examination. Normal cup-disc ratio is about 0.3 to 0.6 depending on the size of the optic discs. When the cup-disc ratio is more than 0.6, this is generally considered to be abnormal and require further investigation. When this is coupled with raised eye pressure, then this is considered to be glaucoma changes on the optic discs that needs treatment to lower the eye pressure. Without treatment, the optic nerve damage will continue and the cup-disc ratio will gradually enlarged over time with result of visual loss. Some patients can develop glaucome-type optic disc changes without raised eye pressure, this is consider to be Normal Pressure Glaucoma meaning that the optic nerve damage happens even when the eye pressures are within normal limits, therefore, treatment or surgery may be require to achieve lower eye pressure to protect the optic nerve.
Optic disc laser imaging
Optic disc imaging is a laser scan that can measure the thickness of the nerve fibre layer surrounding the optic discs. The latest Spectral Domain Optical Coherence Tomography (SD-OCT) can accurately measure the thickness of the nerve fibre layer in micrometres. The newest eye tracking technologies allow accurate scanning of the exact locations as in the previous scans, which allows precise comparison of nerve fibre layer thickness for up to 5% of changes that can be detected accurately.
The picture shows an OCT scan of an optic nerve about one year apart, demonstrating minimal nerve fibre layer thickness changes.